Who knew that needles would bring joy while cotton swabs would instill fear?
When Dr. Erin Bearss talks about the vaccine rollout she led in six Toronto nursing and long-term care homes, she’ll tell you that vaccinating residents was just part of the story. Prior to the January program that saw 1,700 vaccinated, Bearss had spent the previous year swabbing many of the same residents and staff for COVID-19.
Bearss, who had worked as the family medicine residency program director at Mount Sinai Hospital for more than a decade, transitioned to the role of associate chief with colleague Michelle Naimer in April 2020. Tasked with taking on this new role during the early days of a pandemic, Bearss and Naimer created a small committee called the Family Medicine COVID Leadership Team.
“Early on there was a lot of collaboration and we were all figuring it all out together … it was sort of all hands on deck,” she says, adding that at one point the committee was meeting as often as twice a day.
Bearss had noticed a growing number of travellers coming to the emergency room to get swab-tested for COVID-19 as early as March 2020. With the support of Sinai Health Leadership, she set up a separate testing space in one of the Mount Sinai’s administrative areas for the influx of patients requiring tests. At the time, she didn’t realize this would be a trial run for the testing stations she would later set up around the city.
That April, she was assigned to work with nursing homes and retirement and long-care home hybrids to test staff and residents for COVID-19. Since Mount Sinai didn’t have an existing relationship with these facilities, she says a lot of work had to be done to ensure that those living and working at the care homes, as well as hospital staff, were safe.
“The vaccination piece is fun and exciting and happy … the swabbing centers are not that way at all.”
“Most of the time, people are not happy to be there, they’re not happy that you’re telling them they have to isolate (and) they’re not happy when you call to tell them they’re positive,” Bearss says.
Bearss worked to calm general anxieties around testing. If tests revealed bad news, she had to be able to reassure the homes that they would still be taken care of. “What do you do if you swab 100 staff and 90 are positive?” she asks. “So there was some appropriately placed anxiety from the people who worked there.”
As a safety net, Sinai Health helped organize available hospital and temp workers to act as replacements if many the care home staff tested positive. Although there were positive cases, the worst never came to pass.
Dr. Bearss and a few of the hospital’s family doctors and residents were the only ones administering the COVID-19 swab tests at the care homes. But the work and relationship building that Bearss put in at the beginning of the pandemic paved the way for a smooth vaccination rollout when it came time to return to the care homes. Only this time, she had a lot more help.
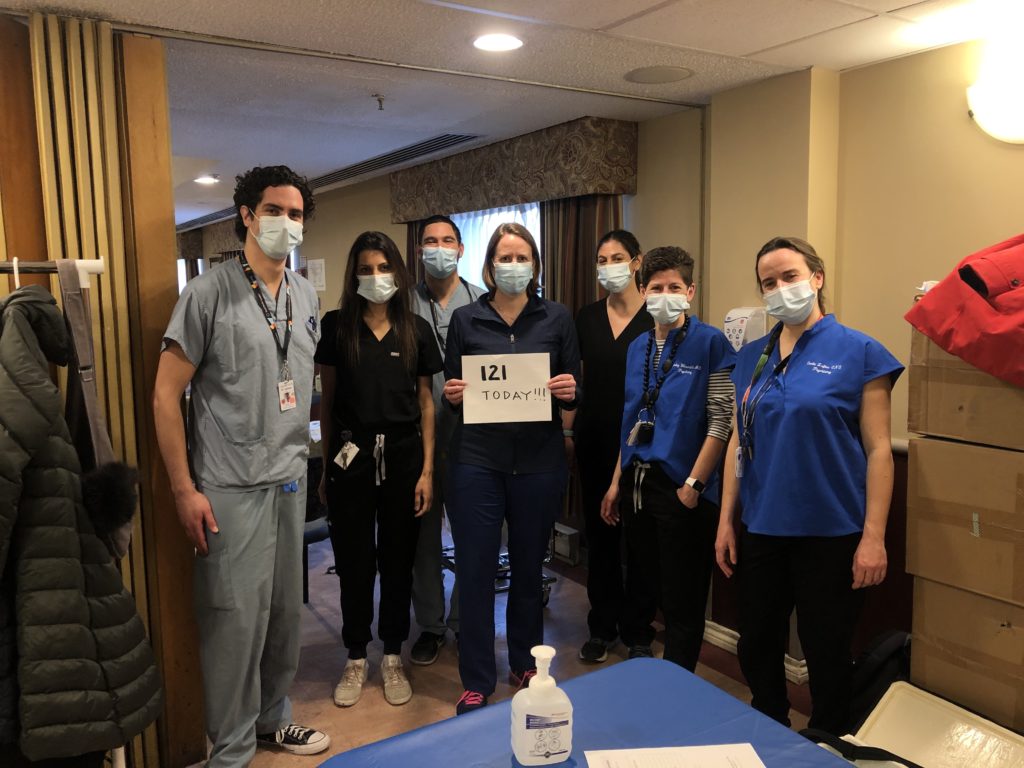
First in January 2021 and then again in February, she coordinated a team of more than 300 doctors from multiple specialties and hospitals to administer vaccines at the same homes.
Bearss remembers one long-term care patient in particular who was being treated by palliative care doctor Ramona Mahtani when she first tested staff and residents. The woman was in her 90s, in poor health and wasn’t expected to make it much longer. But when Bearss returned to the care home in January to vaccinate residents, the same patient was still alive and, with great relief, able to be vaccinated by Mahtani.
“Everybody was in tears,” Bearss said, “What an emotional and meaningful moment this was to have supported this woman, during probably the worst moment of her life, and then to bring that joy and relief of being able to vaccinate her nine months later and really see the positivity in that.”
Who knew needles would bring joy?
In addition to the homes, Bearss was responsible for organizing vaccinations at the ALC Long Term Care/Complex Continuing Care Centre at Mount Sinai Hospital Bridgepoint, the mass vaccination centre at the University of Toronto, and she helped to facilitate the Mount Sinai and U of T pop-up clinic in Rexdale with team lead, Dr. Jasmine Multani. As of June 2021, these two sites had administered a whopping 20,000 and 15,000 vaccines, respectively.
“It feels good, and people are happy, it’s a much more positive and optimistic vibe than we’ve seen in the last year,” says Bearss.
Not your average Bearss
Bearss sees herself as an optimist, who might even have leadership coursing through her veins. Years ago, when her parents spoke with her junior kindergarten teacher, they asked if their little Erin was being bossy with the other students. The teacher replied “No, she’s a leader.”
In her undergraduate studies, she started out in forensic pathology, inspired by Scully from the X-Files. But she moved on to family medicine when she realized she didn’t want to spend all five years of her residency behind a microscope.
During the darkest days of the COVID-19 pandemic, she was struck by how vulnerable she and her colleagues had become.
She says it was a feeling that none of them were used to.
“We in medicine are used to supporting, treating and communicating with people at their most vulnerable stage,” Bearss says. “Usually, we’re fully in control and not the vulnerable ones. I think that’s the difference in this pandemic … It could just as easily be one of us who was getting sick or it could have been one of our family members.”
With this chapter of the pandemic behind us, she says she’s excited to focus on her new role as chief of the Sinai Health Department of Family Medicine without the added pressure of a global pandemic in full swing. But she says there are lessons from this last year that we will carry with us.
“The number of people I’ve gotten to know in different hospitals and different departments – and really feeling like you’re on the same team has really been one of the positive things in the pandemic,” says Bearss. “The Team Vaccine slogan – ‘stronger together’– is a little cheesy but it’s accurate. If we can continue to leverage each other’s strengths and accomplish more together, I think it makes everybody’s life easier and I think the outcome is better.”
She says that there are two main things that she’s looking forward to being able to do again: watching her kids play hockey and traveling.
“One friend said to me that all my regrets in life are travel I didn’t take, and I think that will increasingly be the case. Not just with travel but with things in general,” says Bearss. “I hope that we recognize all of the things we took for granted, some of the appreciation we’ve gained over the pandemic is a bit more lasting … that we don’t fall back into our routines and forget how important those things are and how much we missed them.”
This is one of the first profiles published as part of the Pillars of the Pandemic series – brought to you by the Dalla Lana School of Public Health and Closing the Gap Healthcare. We will release new profiles in the coming weeks, with 13 people being honoured in total.



The comments section is closed.