Rahel Yetbarek sits with her feet up, looking out onto the city and the large swath of treed land that surrounds the freeway below her. The nurse is taking in the view over her lunch break, from the 10th floor rooftop garden at Bridgepoint, a Toronto hospital. Nearby, a few patients do the same. The drone of the highway in the background doesn’t detract from the peacefulness she gets from coming up here.
“I love the view, especially the bridge,” she says, referring to the Bloor Street viaduct. “It’s quiet, relaxing. Most of the time I come here, to read, to eat lunch. At night the view is excellent too.”
Downstairs in the foyer, John Hill, a patient, agrees with her analysis. “It’s a beautiful building – a real Taj Mahal,” he says.
Related articles
- Citizens participate in hospital restructuring processes
- Evidence-based hospital nurse staffing: the challenges
- The challenges of improving hospital food
Like many new hospitals, Bridgepoint is building off of 30 years of research into how design can make patients less likely to get infections, have falls, or be stressed while in hospitals. This evidence-based design has changed everything from the amount of airflow in operating rooms to the view out the window, melding the art of design with the science of medicine. And it has played a key role in how new hospitals like Bridgepoint, Calgary’s South Health Campus and Mississauga’s Trillium Health Centre function for patients and staff.
Evidence-based design
In 1984, Roger Ulrich released a study that looked at patients recovering from gallbladder surgery. Half of them had been assigned to a room with a view of nature, and the other half looked out at a brick wall. It found patients whose windows faced a natural view recovered faster and needed less painkillers. “That’s when the notion of evidence-based design really started to take hold,” says Ellen Taylor, director of research at The Centre for Health Design, a California-based organization that promotes research-driven health-care design. “These are things that maybe we intuitively have known before … but this was the first study that generated that notion that you can document some of these outcomes.”
It has taken a while to get there. Florence Nightingale observed in 1860 that placing patients where they can see out of a window or read by natural light was “quite perceptible in promoting recovery.”
The term evidence-based design was defined in 2003 by Kirk Hamilton, an architect and advocate for evidence-informed health-care buildings. “Over my 30 year career, I’ve designed 15,000 patient rooms,” says Hamilton. “[In the beginning,] I knew an awful lot about those rooms: the size of the window, where the air conditioning system was, the artwork on the walls…but I didn’t know which of those rooms had the lowest rate of patient falls, medication error, infection rates.”
Now more than 1,200 studies have been done on everything from sound muffling to sink design. They’ve formed a framework for thinking about evidence-based design, and some hospital design firms have responded by hiring directors of research and tracking metrics. “Hospitals are just designed differently now than they were 20 years ago,” says Taylor. “It’s pretty much expected at this point that your design team is bringing that level of knowledge.”
Reducing stress to boost healing
Ulrich’s legacy is evident in newer hospitals’ focus on what’s outside patients’ windows.
“The first thing patients mention is the view,” says Celeste Alvaro, researcher at the Bridgepoint Collaboratory for Research and Innovation, which is studying the impact of the new building. “It’s increasing their comfort level, but it’s also increasing their sense that they’re in a place of wellness.” Alvaro’s team has found that any meaningful view – including one of the cityscape – is beneficial, not just those of nature. And it’s not just patients that are helped: “what’s good for the patient is good for the staff,” says Gregory Colucci, the architectural lead on Bridgepoint.

Bridgepoint’s windows are meant to mirror patients coming into a hospital horizontal, on a stretcher, then becoming vertical as they heal. Bedroom photo and rooftop photo (top), both Tom Arban.
Natural light, a view, accommodating family, and giving patients control of their own lighting can all help lower stress. That’s one reason why large, light-filled entranceways, more reminiscent of shopping malls than hospitals, greet patients in newer builds. Calgary’s South Health Campus features multiple-storey high floor-to-ceiling glass to reduce stress levels right from when patients enter the building. Facilities like a YMCA in the hospital increase the feeling that it’s part of the community.
Bridgepoint is also designed to encourage socializing, with a dining room on each floor, patient lounges, a green roof and outdoor eating area. Creating a sense of connection works as a buffer against the stress of being in hospital. That’s particularly important for its unique patient population – the average Bridgepoint patient has five complex health conditions, needs rehabilitation, and is in their mid-60s.
Including public input from the planning stages is crucial to success. At the Alberta Children’s Hospital, that step even included the kids. “We engaged a group of architects. and they drew up what was in their minds a lovely building,” says Lois Ward, site director at the hospital. “We showed it to a few kids, and they absolutely hated it.”
Thanks to their input, the hospital now looks like something a kid dreamed up, with a green, yellow and blue exterior and two-floor high window frames that make the building look smaller and more welcoming. More practical changes at the hospital included adding built-in beds to patient rooms, so family members can stay over, as well as storage units for them to hang their things.
The South Health Campus also included input from a patient and family advisory council. The process recently won accolades from the U.S. Institute for Patient- and Family-Centered Care. New patient-centered rules include differentiating between when primary family members or support people are allowed to visit (24/7) and regular visitors (only during visiting hours).
The single-room solution
Another thing you’re far more likely to find in newer hospitals? Private rooms. “The hottest topic in health-care delivery is single rooms,” says Karen Stockton, who has consulted on several hospital designs and is a clinical director at the Ottawa Hospital. In Calgary’s new South Health Campus, 90% of the inpatient rooms are private rooms. They also include a bed area for family members to stay over.
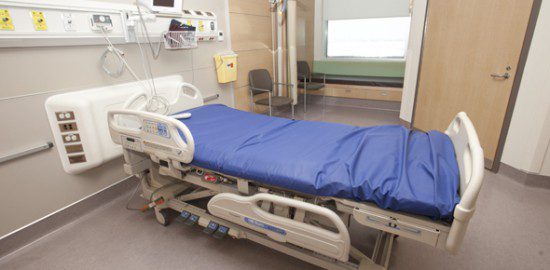
South Health Campus patient feature beds for visitors nestled against the windows, with a blind for privacy beside them.
Private rooms, especially those with bathrooms, are one of the most important infection control steps. That was highlighted in the SARS crisis, as multi-bed ER and ICU rooms increased the rates of infection. Single rooms are also the single best way to improve many outcomes, including falls, medical errors, quality of sleep, patient satisfaction and stress levels in both patients and staff. However, there is some financial concern around them, as hospitals built with only single-bed rooms would likely lose the ability to charge for them.
Mississauga’s Trillium Health Centre’s new wing also increased the number of private rooms, as well as adding a sink for health care providers near beds in every room, and alcohol dispensers in the hallways. A post-building study found staff in the new wing were more likely to comply with proper hand hygiene, and there was a decrease in the number of infections as well.
In addition, better designed hallways, single bathrooms, good waste management systems, and easy-to-clean materials help lower infection rates. Modern hospitals also have more frequent air exchange rates than older ones do.
These all add up to good news for patients. “[20 years ago,] issues such as hospital acquired infection were not even addressed through design and construction standards,” says Rita Mezei, executive director at the Canadian Centre for Healthcare Facilities. “Today, there are national and provincial standards of practice around it.”
Keeping pace with technology
It’s hard for hospitals to keep up with changing standards and technology, with some even having to change plans mid-way through the building process as a result. “It’s like buying a computer – you go out and buy a computer, and a year later somebody says you need a new computer,” says David Johnstone, who was clinical director of the Mazankowski Alberta Heart Institute from 2006 to 2011.
Hospitals are now more IT-focused, and new buildings support wireless systems and online medical records with more cables in the walls and WiFi. The rise in same-day surgeries and laparoscopic surgery also affects the number of patient rooms needed and the design of ORs.
The Mazankowski clinic anticipated those needs with a hybrid OR that can be used for minimally invasive surgery. But some other technology it chose didn’t work out as well. TVs with washable keyboards were ordered so doctors could show educational video clips to patients. The hospital hoped patients would also use them to educate themselves on their condition. But patients don’t seem interested in that during the four or five days they’re in hospital enduring the acute phase of recovery.
Focusing on more generic design principles, operations and workflow can help dodge some of the issues that come up with changing technology, says Stockton. “Some things don’t change as fast as others, like the [role of] frontline providers. If you build the majority around that, you should get the majority right.”
‘How do we know our success if we can’t measure it?’
It’s not enough to build based on evidence; new hospitals should also be objectively evaluated after they start treating patients. This last step is where many falter.
“How do we know our success if we can’t measure it?” says Mezei. “Unfortunately after building a multi-million or billion dollar project with public funds, there is no requirement to document and share the things done well and the things done wrong.”
Post-occupancy evaluations should be a collaborative effort. “When we are talking about studying the interaction of people, place and process as an outcome in a critical environment such as a healthcare facility, you really need to bring all the experts together,” says Terri Zborowsky, a research associate at the Centre for Health Design. That includes the architects and engineers, staff and a health-care researcher, working towards objective results. “We really encourage depth and rigor in this area, so we can properly grow our knowledge base,” she says.
Bridgepoint is in the middle of the largest post-building analysis in Canada. It looks at health outcomes, but the focus is on psychological benefits: “the collection of design features that would eliminate the psychological obstacles to healing, boost spirits and morale and motivate patients to re-engage in life,” as the preliminary reports puts it. The’re looking at things like length of stay, depressive symptoms and sense of belonging from patients.
The analysis is possible because they have two control sites – the old facility, where they began interviewing patients, and the nearby West Park Healthcare Centre. “You really need to have a comparison point to the earlier hospital, or the most closely matched facility,” says Alvaro. “Otherwise you really don’t have any ability to attribute observed outcomes to design.”
Her research has uncovered some surprises: some design features, like patient lounges and terraces, weren’t being used as much as expected. At the same time, people reported they felt inspired by transition zones, like the seating areas and the entrance.
“This environment is having a positive impact,” says the architect Colucci. “Architecture does not provide a cure, but it can enhance the quality of care.”




The comments section is closed.
Increasing awareness of the harmful qualities of artificial light (too much blue, unbalanced) and non-native EMF (not good for anyone, much less patients with heath challenges) will hopefully evolve hospital design even more in the future, and feature strong grounding solutions, windows that open fully to allow more natural light to come in, patient rooms oriented to the east for the all-important daily setting of the circadian rhythm, plenty of outdoor spaces for patients to spend part of their day, and supplemental infrared, amber and uv light indoors to compensate for the balanced spectrum lost through glass and by the lighting needed 24/7 for patient care.
Great piece. The linkage between design and health outcomes seems intuitive, but emerging support from large-scale studies speaks volumes to the decision-makers behind hospital redevelopment.
I’ll pose the following point. In this environment of activity-based funding the definition of a hospital is rapidly changing. One of the outcomes of the new funding model is to create centres of excellence and defined ambulatory settings, which may shift volumes towards the community and throughout LHINs.
%featured%While the relationship between inpatient outcomes and design is becoming more established, how can hospitals rationalize capital-intensive design initiatives when their respective model of care is in a state of flux?%featured% Further, if hospitals without deep pockets or comprehensive fundraising infrastructure cannot ascribe to the ‘gold standard’ of design, are we not creating a two-tier system?
Excellent point Navin – the models between building and delivery certainly don’t appear to be on the same path. %featured%I also note the amount going into building acute acre hospitals or updating them but see very little investment in long-term/chronic care beds yet we know there is a great need there %featured%– be interesting to see the actual figures on numbers of beds in acute care that are occupied by patients waiting for long-term or chronic care.
I also feel the view re infections is a little short-sighted. Yes, hospitals regard the payment difference from ward to semi or private coverage as a “cash cow” (much like the parking lots/garages) but how much is gained when you have increasing amounts of both C diff and MRSA and all of those patients require isolation? To say nothing of the risk to other patients exposed while staff waits for lab tests to confirm infection? Somewhat like shutting the barn door after the horse hs bolted.