In many provinces across Canada the authority and governance of health care has been moved to regional authorities, based on the belief that local authorities can better integrate and coordinate services, and contain costs.
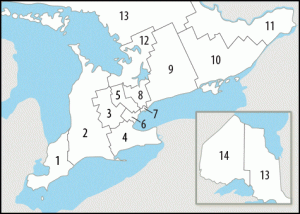
Ontario created 14 Local Health Integration Networks (LHINs) in 2006, with the mandate to plan, fund and integrate health care services for more efficient care in their regions.
However, the ability of LHINs to deliver on their mandate and improve health care in Ontario has come under fire, and the future of the LHINs is a major issue in Ontario’s 2011 provincial election.
The future of the LHINs has been a central item of opposition party platforms in Ontario’s upcoming October 2011 election. The Progressive Conservative Party platform includes a promise to eliminate Ontario’s 14 LHINs as does the NDP platform which promises to “scrap the LHINs and replace them with effective local decision making.” The total budget to administer Ontario’s 14 LHINs is $68 million, a small fraction of the $44 billion spent in 2010 on health care in Ontario. A recent series in the Hamilton Spectator notes that moving the LHIN administrative budget to front line care could “pay for 154,420 consultations with a cardiologist, 291,500 abdominal MRI scans and 494,000 basic CT scans of the head.”
Would eliminating the LHINs lead to more front line care? If the LHINs are eliminated, who will administer and manage the health system?
Ontario: A province like no other
As the cost and complexity of health care delivery systems have increased, there has been a movement across Canada to develop regional structures for the governance and administration of health care provider organizations, to better integrate services. By the end of the 1990s all provinces in Canada, with the exception of Ontario, had created regional health care authorities.
Ontario has taken a cautious approach to regionalization. About ten years after regionalization of health care governance occurred elsewhere in Canada, Ontario passed legislation for LHINs in 2006 , creating 14 health regions.
Managing and administering a complex health care system whose annual budget exceeds $40 billion is a mammoth task. Many argue that LHINs were not given sufficient authority to meaningfully fulfill their mandate. A recent commentary argued that “the LHINs have been and are set up to fail” as they only have about 30 employees each, compared to the nearly 4000 Ministry of Health and Long-Term Care employees.
LHINs technically have authority over more than $20 billion in funding to health care organizations such as hospitals and community care access centers. In reality, however, LHIN administrators have little say in how these funds are distributed, and the money itself flows directly from the government to hospitals and other health care providers. In other provinces, health authorities receive money based on the population they serve and have the authority to make decisions on how and where to direct funding. While a new funding formula is meant to help improve population funding based on need Ontario is still far from a population, needs based approach.
Unlike other provinces, when the LHINs were established, Ontario chose to retain boards for individual hospitals and other local health organizations. Some see this as a major impediment to change, because powerful hospital administrators and boards sometimes work against LHIN efforts to rationalize and integrate services. Chris Carruthers, a retired Ottawa orthopaedic surgeon and former Chief of Staff of the Ottawa Hospital says that “Ontario is unique in Canada for leaving hospital boards in place” in a regionalized system, and that strong hospital governance has “been an impediment to quick decision making and collective integrated care” by the LHINs. Carruthers says that retaining hospital boards means “LHINs don’t have the power to improve services across their regions,” depriving them of the ability “to make tough decisions about integrating care.”
LHINs have the mandate to plan, fund and integrate hospital, home and community services. However, like other health regions in Canada they lack responsibility for primary care services, pharmaceuticals and other complex provincial programs like cancer and transplantation. Malcolm Maxwell, President and CEO of Grand River Hospital says that Ontario’s health system is a product of a hospital-based insurance system which is not “effectively integrated with primary care and Community Care Access Centres”. Unlike other provinces, LHIN’s mandate does not include the management of public health offices and agencies, making integrated health planning with public health challenging, especially during outbreaks like the 2009 H1N1 influenza pandemic.
The politics of LHINs
LHINs have legislative authority to restructure, merge, and close facilities within their regions. However their ability to make major changes to the health system has been limited. Restructuring decisions can be highly unpopular with communities and are politically charged. However, the logic behind created local governance for health care is that local bodies will be better able to understand communities when making these choices. LHIN legislation outlines the importance of transparency and public accountability during these often painful decision making processes. However, some LHINs have come under fire for a lack of transparency. The Niagara Haldimand Brant LHIN was the subject of a highly critical report by Ontario’s Ombudsman which described a lack of community engagement during a controversial hospital restructuring process.
In spite of some successes in leading the difficult work on health care integration and restructuring, the LHINs have been publicly criticized as an additional, costly layer of bureaucracy within the health care system. They have been blasted by critics in Ontario’s legislature as a “bloated bureaucracy” that is “out of control” and “need[s] to be reined in.” Some critics have called for the LHINs to be scrapped entirely.
But who will step in if the LHINs are abolished? Who will administer and manage the quality and performance of the health care system?
Dr. Wilbert Keon, a retired cardiac surgeon and senator, and current chair of the Champlain LHIN board, is concerned that changes to the current regional structure will create challenges, suggesting that “we had a decade of anarchy because one system was taken out of play and it has taken a decade to replace it.” Keon says that political interference with health system governance is “the price we pay for democracy”, but that it has created “a stop and go system” where changes are made based on politics, without sufficient consideration for the performance of the health care system.
Strengthening regional governance for health care improvement
With a provincial election on the horizon in Ontario, any incoming government will continue to struggle with managing health expenditure growth while improving health outcomes for Ontarians. Maxwell suggests that “it is difficult for 130 odd free standing hospitals in Ontario to independently develop and apply clinical performance measures.” So, while it may sound appealing to suggest LHIN budgets should be converted to “front line care”, Ontario’s delivery system currently is short on strong management at the regional level. Ontario’s geography is vast, and there are large service integration and quality challenges which can only be met by some form of regional oversight, coordination and governance.
No matter what system is put in place, leading practices from other health regions suggest that regional bodies should be required to publicly report on the quality of care they provide and on the health of the population they serve, using a set of metrics that is common across the province
Ontario has many challenges to drive improvements in health care performance, management and governance in the coming years. Do you think that LHINs have the correct structure and mandate to help achieve this?


The comments section is closed.
Well written summary of the key issues. the LHINs of 2006 were an intermediate step to true regionalization, we need to think about a LHINS 2.0 Strategy. The issue of still having hospitals boards is I think a critical impediment to the effectiveness of the LHINs and I agree with a previous poster – one that needs be elevated in the public discourse on the topic. Here’s an idea: A) take the top 2-3, best, most effective hospital board directors from each LHIN hospital send them to form a new LHIN board. B) Remove/shut down hospital boards and remove/refresh the current LHIN board.
With $0.49 of every tax dollar going to health care and a shrinking tax base as the baby boomers retire, and a greater demand for health care as this same group ages, solutions to streamline must happen.
The LHINs can’t touch issues of waste and duplication between neighbouring communities.
In my community I see millions of wasted duplication because various health services don’t share resources and because a hospital corporation or hospital foundation in one city wants “their” hospital to have a new CT scanner or mammography machine even though there is one twenty minutes away that is not being used to anywhere near capacity.
Another example is proximity of many tertiary services next to hospitals that don’t share services because they are separate corporations, yet all draw from the same tax payer purse. A long term care facility doesn’t share food services or maintenance with the hospital next to it. Yet they could streamline and save massive amounts of cash if they did.
The system will go bankrupt, we will lose service, and yet there is no one to prevent millions in waste in a communities of less than 100,000 people.
Most of us take this system for granted without really understanding how it works and why it is broken. We are fortunate to have some of the best health care in the world, but the current model is not sustainable.
I’m very impressed by this article; highly informative yet succinct and I’m glad this issue was brought up to the public’s attention.
Yes, for the most part, I do agree with the comments below. LHINs are long-term investments; right now, it’s slightly too early to measure the gains and judge whether or not to ‘scrap’ it or not. For that reason, I found it utterly absurd that the PC and NDP parties are thinking of getting rid of it completely, if elected. To me, that’s ignorance on their behalf. Instead of trying their best to improve the current situation, all they plan to do is obliterate it and pretend as if LHINs never existed before.
As Peter and Don alluded to, I believe it’s important that leaders of a higher caliber serve on the boards of LHINs. I agree that right now, LHINs are not able to operate at its full efficacy due to the unduly overpowering control the hospital boards have on the governance of our health care system. So, I think there needs to be greater incentives set in place to attract highly competent community/business leaders to the boards of LHIN – only then will Ontarians will see the benefits of an integrated health care.
The LHINs do not have Authority of Regional Health Authorities in other provinces to accept patient complaints about hospitals and investigate them.
Hospital autonomy doesn’t work for patients because it allows hospitals to deal with patient complaints internally without patient appeal. One example of how this failed was the Native man who was beaten up by the security guards at St. Mike’s hospital while they hurled racial epithets at him. It turns out there had been other complaints about their security and that the hospital had dealt with them internally. Nothing changed until the hospital was embarrassed in the press. We need external review of patient complaints, as soon as possible.
We also need a fully transparent regional system which is held accountable with legal sanctions if it fails to represent the public interest.
Your article outlines many of the arguments very well, but there should have been another option on the survey:
Do you think that LHINs have the right structure and mandate?
No, the current LHIN structure fails to hold hospitals accountable for patient complaints, fails to meet the needs of some of the communities over which they have jurisdiction, and has had numerous scandals which suggest they don’t know how to manage their money. Please replace them with a system that is fully transparent and accountable and has sufficient oversight over hospitals to protect the interests of patients and the public.
Ok, you could shorten it. But I couldn’t fit that view into any of the options you provided. The last option assumes that LHINs are fixable. Are they?
If the LHINs were really the answer to greater hospital transparency and accountability, maybe they would have opposed the hospital secrecy clause of the freedom of information act, which passed this May. They could have demanded that hospitals make all quality of care information public, with obvious protection for personal health information. But they were publicly silent on the matter.
An important topic and a well presented précis of the issues. But there is some simplification at hand. While I agree that it was/is a mistake to leave the hospital boards in place while installing the LHIN governance, it would be a mistake to abolish one or the other and expect violent agreement to break out around the province. Hospital boards are influential and articulate voices for their own interests – as they are supposed to be – and LHINs struggle to navigate the ‘system’ to common objectives. Necessarily at times, the interests are pitched against each other. I would argue that powerful hospital boards get in the way of much needed systems thinking and planning and so LHINs need to have much more clout and leverage to develop and manage the healthcare system. That said, the quality of board leadership at the LHIN level needs to become as prestigious and as influential as that currently in place at the hospital and the LHIN board needs to be populated with citizens of the highest calibre, not unlike what we have in the best hospital boards. Governance and stewardship issues will be central to future success. The LHINs then need to have more discretion over the budgets and services for which they are responsible. Finally, I agree with Don Taylor that this is a long game, not one where we will see big gains in the immediate term.
No one is suggesting that removal of hospital boards is going to fix every problem in the system. I agree completely that LHINs will need improved leadership, not just at the board level, but in their executive and support staff. Indeed, no one familiar with healthcare governance would suggest that LHINs could, without a significant increase in capacity, suddenly operate at the level of health authorities elsewhere in the country. Here too it is instructive to see how other provinces approached regionalization. In BC, regionalization occurred in two steps, first the hospital boards were removed in favor of 54 regional authorities. Then the 54 were whittled down to 5 regional authorities and one province wide authority (responsible for maternal health, cancer, renal, etc). At each stage, a number of directors and staff were carried forward from the old organizations, preserving valuable experience and institutional memory. Indeed, one of the benefits of shrinking the number of boards was that the talent pool of directors became a great deal deeper (particularly important in the world of competency based boards).
However, none of this changes the fact that the currently political dialogue has provided the public with only two options: scrap LHINs or maintain the status quo. This is a false dilemma. There are other choices and it’s great to see Health Debate draw one of these into such sharp focus. Unless more follow suit and push to get this option into the public debate, we risk taking an enormous step backwards.
This article highlights the issues succinctly. I don’t know whether or not the LHINs have too little clout or are ineffective. I do know this, though:
1. Regional integration is happening. Our two Mississauga hospitals are actively exploring a merger, with the support and encouragement of our Mississauga-Halton LHIN. And are already integrating the two hospitals’ human resource and MRI functions, one big benefit of which is an equalization of MRI wait times. Now that’s improved fairness and access.
2. Large scale systemic change takes considerable time – 6 to 10 years. Most LHINs didn’t really get fully up and running until 2008. So it likely is premature to assess their effectiveness.
3. Monolithic organizations and a system of fragmented local organizations are equally inefficient and ineffective. LHINs seem to offer a more balanced approach.
An excellent piece. The problem of Ontario not having eliminated hospital boards when it introduced LHINs has received far too little attention in the press or in political dialogue. Very happy to finally see the problem described so well.
It is indeed wasteful to have two levels of governance working against each other, but it’s fascinating that political parties and pundits have focused so intently on doing away with LHINs, rather than doing away with hospital boards, which every other province found to be more cumbersome and wasteful. It’s interesting that we often hear about the $68 million that LHINs are costing us, but no one seems to have checked to see how much having 130 different hospital boards is costing the system.
Not dealing with the boards was a huge mistake, but then hospital board appointments are prestigious and no one wanted to deal with the political fallout of firing a thousand board members, all community or business leaders. Something clearly has to give, but the proposal from opposition parties to just scrap the LHINs is reckless. Far better would be to show some courage, stand up to the hospital boards who have actively stood in the way of LHINs pursuing their mandate, and disband them. Only then will Ontario stop lagging a decade behind the rest of the country in healthcare governance.
Since I live and work in Toronto, all my health care needs should be available where I live – since the LHIN’s have been introduced, Toronto has been divided into 5 LHINs making health care in Toronto inequitable in the least and discriminatory in the worst. I am located in Central LHIN and wish to know what I have in common with the people of King City or Kleinberg or even the farmers who live in and amongst the estates scattered throughout the north part. I have a lot more in common with the working class community in Toronto then a middle class one in Vaughan.
When being sent to Etobicoke Hospital which takes about 15 minutes to drive and is located in Central West LHIN, a world of difference in the amount of services between Central LHIN abounds – how is this equitable?