While on call on the internal medicine service at my hospital, I recently admitted a 47-year old woman overnight, who had increased swelling in her ankles and a fluid collection in her abdomen. After taking a thorough clinical history and performing a complete physical examination, I presumed the cause to be alcoholic liver cirrhosis.
I remembered seeing similar patients as a medical student, and observing the residents supervising me at that time order a battery of tests to ‘rule out’ all other causes of liver cirrhosis. Trying to be a ‘thorough’ physician, I emulated this ‘shotgun’ approach to ordering diagnostic tests for my patient with liver cirrhosis, including an echocardiogram, since heart failure is included on the list of possible causes. I had hoped my staff would be proud of me in the morning that I had provided such comprehensive care for my patient – he was not.
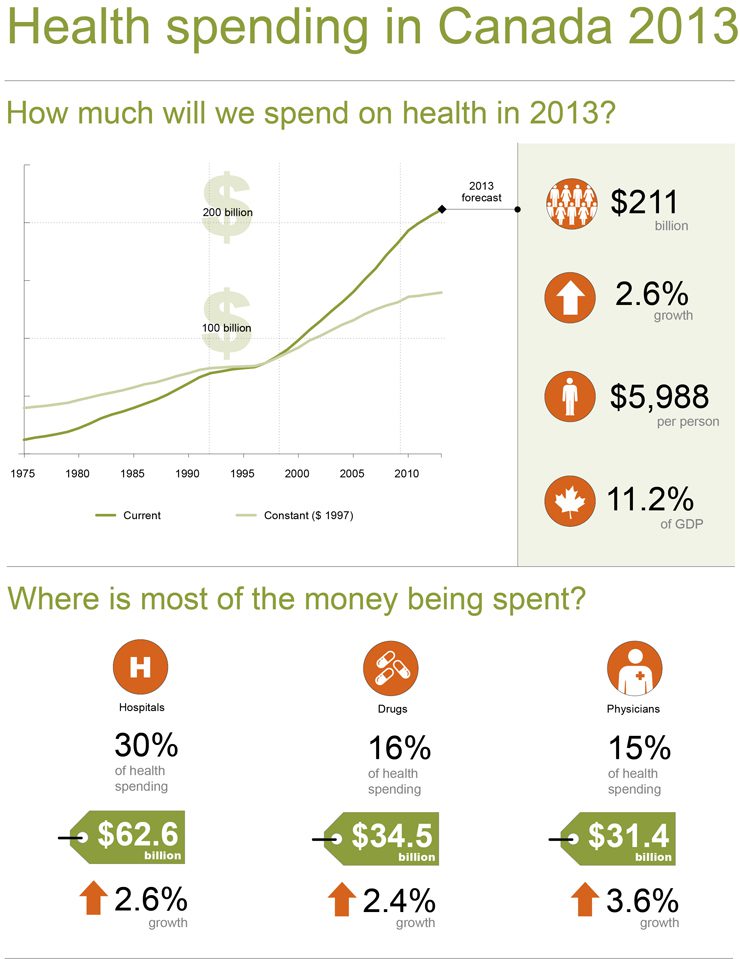
Diagnostic testing, and medical imaging in particular, is becoming increasingly easy for physicians to order . At the same time, the cost of providing care is rising (of course the rise in healthcare costs is multifactorial, with diagnostic testing only one component of total healthcare costs). According to a recent report from the Canadian Institutes for Health Information, the growth in Canada’s total health expenditure increased by an average of $9.2 billion yearly. Canadians now spend $5802/person on healthcare (up from $3213/person in 2000), which accounts for approximately 11% of Canada’s gross domestic product, 40% of provincial budgets, and exceeds the rate of economic growth over the same time period.
Providing cost effective care is challenging, especially given physicians’ discomfort with diagnostic uncertainty. Traditionally, medical students have been taught to create a differential diagnosis of diseases for a patient’s clinical presentation and then address each of these items in a systematic way to eliminate them from their list.
This strategy of ‘shotgun testing’ has been demonstrated by Calderon and his colleagues to be an expensive and ineffective approach to patient care. They examined how effective diagnostic tests (postural vitals, cardiac enzymes, ECGs, telemetry, echocardiograms, electroencephalograms and head CTs) were when routinely ordered to identify the cause of fainting (known as syncope) in elderly patients. The simplest and cheapest test was also the most infrequently ordered (postural vitals; $5/test ordered in 38% of the cases), but the most effective in determining the cause (15%). Compare this to head CTs that were ordered 63% of the time, cost ~$1500/test and only identified the cause 0.5% of the time, never mind the radiation to which these patients were exposed. Yet in the emergency room, I can get a head CT for my elderly patient presenting with a fall as easily as I can get a set of postural vitals!
Thankfully, many thoughtful physicians (including my disappointed staff the next morning) are trying to shift our focus to obtaining valuable information and making responsible decisions with our test ordering. The Choosing Wisely campaign”focuses on encouraging physicians, patients and other health care stakeholders to think and talk about medical tests and procedures that may be unnecessary, and in some instances can cause harm.“ It publishes a list of evidence-based recommendations aimed at ensuring the most appropriate care is individualized to patients, with the hope that they will stimulate discussion about the need—or lack thereof—for many frequently ordered tests or treatments.
For the evaluation of syncope, the American College of Physicians’ Choosing Wisely recommendation is to avoid obtaining brain-imaging studies unless there is an abnormality in their history and physical exam to suggest otherwise – a recommendation supported by Dr. Calderon’s study.
In the case of my patient with alcoholic cirrhosis, unfortunately there was no Choosing Wisely list to tell me what to do (or what not to do!). But I learned a valuable lesson in listening to her, performing a thorough physical exam and heeding the advice of my staff – to utilize good clinical reasoning with regards to her care and avoid ordering tests to rule out diseases that my patient had very little probability of having based on my initial interactions with her. She knew why her liver was damaged; what she really wanted was sound medical advice in how to manage her disease going forward.
So I cancelled the echocardiogram, saved my patient the trouble of an unnecessary test and hopefully saved the system a few bucks at the same time.


The comments section is closed.
For anyone interested, Dr. Wendy Levinson has published an interesting commentary on the Choosing Wisely campaign coming to Canada. It can be found here:
http://www.cmaj.ca/content/early/2014/02/18/cmaj.131674
Kieran, thank you for the thoughtful piece on the your clinical experience and the importance of resource stewardship in medical education! As a fellow medical trainee, I completely agree that this topic needs to be taught from the very beginning of medical education.
It is important to emphasize that Choosing Wisely and the stewardship movement do not revolve around cost, but rather the potential harms of overuse to the patient and health care system as a whole. While physicians always strive to provide the best possible care to their patient, sometimes medicine’s hidden curriculum perpetuates many unhealthy habits such as ordering to satisfy curiosity, impress an attending, or simply lack of better knowledge. As Ms. Whitehead points out patients have no desire for the unnecessary stress, wait times, and potential harms (or false positives) of a test or treatment that will not impact their care. By teaching stewardship awareness from the very beginning of medical education, students will be equipped with knowledge to combat the hidden curriculum, reduce harm to patients, and potentially even lower overall cost to the healthcare system.
Thanks to a very supportive administration, the University of Toronto has been integrating discussions of stewardship into their undergraduate medical curriculum. No upheavals of curricula or additional lectures were needed; instead by simply changing discussions from “What tests could you order?” to “What information will this test give you and how will that information impact your patient’s care?”, medical students can begin to incorporate appropriateness into their decision-making process. In the past few months, it’s been incredible to see students’ awareness of stewardship grow and the beginning of what I hope will be a shift in the culture of medicine.
Consideration of cost has no place in the physician thought process. if a physician deems an intervention to be nevessary, it should be based on clinical judgment and whatever unbiased evidence is available. Cost is irrelevant.
I worry that, much like the deprofessionalization of medicine that is insidiously being indoctrinated upon medical students in theform of equating allied health workers with physicians, the notion of considering the cost to the system is similarly being put on young doctors as as important a consideration as patient care itself.
If the system cannot sustain medical practice, cost cutting could begin by paring down the overcompensated administrator positions(there is a vp for everything) rather than cutting into direct patient care cost.
Thank you for the insightful comments Dr. Glover. While I agree that interventions should be considered on the level of clinical judgement and the use of high quality evidence to guide those decisions, the doctrine of cost is merely one of many avenues used to help trainees consider the importance of their clinical decision (much as the actual process of moving patients in hospital from their bed to the testing location – a factor many of us do not consider at all but can be quite distressing for our patients).
Choosing Wisely aims to create exactly the discussion between patients and their physicians that you are encouraging – are the interventions we as clinicians are ordering necessary?
Take for example the patient with advanced dementia who is fully dependent on all ADLs who is suspected to have a PE – a CTPA may be clinically “necessary” to diagnose the disease entity, but does it provide valuable care to our patient?
There are inherent risks and ‘costs’ to our patients in performing such an intervention (renal injury, radiation exposure etc), but also a cost to the system that should be considered as healthcare custodians.
No one could argue that a CTPA is necessary to diagnose the PE, but I would argue the talents of the clinician comes in their value judgements for their patients which can be supported (but not indicated) by framing it in the context of clinical restraint.
I believe both trainees and clinicians should be aware of the cost, effectiveness, indications and limitations for diagnostic testing as mentioned by Dr. Quinn.
I worry though that such efforts to curb or criticize supposedly inappropriate or wasteful use of such diagnostic tests is painted in too simplistic terms, which does not reflect the uncertain, complex and ever-changing presentations of patient’s symptoms in emergency rooms, hospital wards and doctor’s offices.
The article brought to mind the excellent introspective novel “How Doctors Think” by Dr. Jerome Groopman, in which the author reviews case studies where expert, well-intentioned clinicians fell victim to logical fallacies which lead to poorer care for their patients.
One such cognitive error that comes to mind when discussing the underuse of postural vitals in the workup of syncope is the risk of “satisfaction of search”. The cognitive error of satisfaction of search consists of the tendency to make a diagnosis immediately, effectively ending the diagnostic process, based on the first positive test or sign of disease found.
While it sounds like postural vitals are inexpensive, effective and underutilized, I do worry that relying on them alone will lead to this cognitive error of “first diagnosis”, as orthostatic hypotension is common, benign but also likely comorbid with other more serious conditions. Given that orthostatic hypotension itself is more of a clinical sign than a true diagnosis with a wide differential diagnosis behind its underlying dysfunction, criticizing physicians for not using the “simple” or “cheap” test at the macro level seems to miss the complexity and obligation of serving the individual patient.
We should all take pause and reflect on why we are ordering tests, if it will it benefit our patient, understand the limitations and risks of the tests we order, discuss these limitations with our patients and decide if test results will indeed change management. Studies like those from Calderon et al are helpful in making us take pause and reflect on our approach, but my experience is that many cases in the everyday clinical practice don’t fit very well into algorithmic care and can’t substitute for clinical judgment, which as Dr. Groopman unfortunately suggests, is prone to many pitfalls in and of itself.
Most patients have no desire to endure tests that are unnecessary. However you do not want Canadian doctors crossing over in to the mindset of determining the need for a test based on cost, doing so could cost the patient harm & the physician disciplinary or legal actions.
If a patient has an extensive medical history they are one of the quickest & most effective ways of determining the need for tests in ongoing treatment. At times I have seen physicians ignore or worse still fail to give the patient the opportunity to give a detailed history. In these cases it appears that in order to save on the investment of their time they instead choose multiple tests simply because they are available, easy & frees up the physician to keep the revolving door of patients moving. The other consequence of this practise (& at higher costs) is that it drags out the patients diagnosis & course of treatment. For example you wait for the appointment for the test, you wait for the report to be completed & sent to the doctor, you then have to wait to get back in & see the doctor. In many cases you are than referred to a specialist that you wait months to see. The specialist may order additional test & even refer to another specialist for a second opinion. Finally you often have to wait for treatment, especially if it requires surgery.
The system needs to find a balance instead of swinging the pendulum from one extreme to another. Both doctors & patients need to find better ways to communicate, to learn how to actively listen & seek diagnosis & treatment with common sense.
histories are not sought to tne extent they should be due to a combination of time pressure and an overvaluing of procedural services relative to history and physical examination.
if the h&pwere valued more, we would see more extensive histories and a lower reliance on procedures and tests.
Thanks for your piece, Kieran! As a response to ever-proliferating medical technologies, the Choosing Wisely campaign has done a lot to encourage and inform conversations about how we can make medical care more thoughtful. It’s important for trainees like ourselves to reflect upon such philosophies of care and consider how to structure our own clinical practice. My belief is that such conversations should be about patients first (ie. whether or not the proposed test or intervention is actually contributing to their care) and about costs second. Your article is a great example of this. Residency offers us a great opportunity to become expert clinicians, which means knowing when and when not to order the echocardiogram.
Costs should not be considered at all. We fail to realize that there are other areas in the health care system that could be pared down before even considering patient care cost.
Fortunately, my current supervising staff is also a model of clinical restraint. See his excellent commentary in JAMA on the issue here:
http://jama.jamanetwork.com/article.aspx?articleid=1367571
Congratulations on such a thoughtful piece Kieran. I think there is opportunity to build the “choosing wisely” mindset into our hospitals in a much more deliberate way. Standards like this are being adopted through Open Source Order Sets, Choosing Wisely Canada ( coming soon!) and even the Quality Based Procedures that are part of new hospital funding models. As I hospital CEO I welcome these initiatives as long as there has been active involvement of clinicians in their design. But how do we get over the hurdle that this is seen by many physicians “cookbook medicine/” or unnecessary control over their independent practice and prerogative? Welcome your thoughts, Thanks, Leslee
Hi Leslee,
Thank you for the kind words and your interest in my piece. After reading Dr. Detsky’s piece on the same issue, I have come to the conclusion that the answer lies in changing the culture of medical education from the beginning.
We need to learn to reward restraint (in addition to a comprehensive medical knowledge of diseases and their treatment possibilities) in our medical trainees and recognize it when it is practiced. This should happen from day 1 in medical school and continue throughout our medical training.
I have also come to learn about alternate funding models that provide a standard monetary amount for ‘packages of care’. In this way, physicians and the medical staff receive a lump sum for a single medical issue (e.g. heart failure admission) and if the team can provide care for less than that value (the obvious challenge being to maintain an excellent quality of care – one that can be paradoxically compromised through over investigation anyway) then the extra funding is theirs to keep. Determining what is an appropriate amount has its own problems, but one that could ostensibly be determined through careful study across the nation on average costs. Care that overruns this cost must be then provided at the expense of the medical team (i.e. No further billing for days in hospital).
While this solution is ripe with issues in itself, it demonstrates the need for a multifaceted approach: one that encompasses interventions in medical education and healthcare funding among others.
Nicely said Kieran. This is more than trying to save a buck here or there, or this test vs that. It is ultimately about something bigger, which is changing the culture…of medical education, clinical practice and patient expectations. More is not necessarily better.
We at Choosing Wisely Canada (follow us @choosewiselyCA) are fortunate to be working with the CMA, and 28 Canadian national specialty societies to develop lists of “Five Things Physicians and Patients Should Question.” The first 8 of these lists will be launched in April 2014, with the rest to follow. In addition to coming up with these lists, we are working with a variety of groups to ensure that they are implemented and become part of the health system’s collective consciousness. Thoughtful pieces like yours adds to the important conversation that we hope will continue to grow.