Canada’s most popular over-the-counter ointments for wound treatment are like “poison ivy in a tube,” dermatologists warn, and are the most common medical substances causing allergic contact dermatitis (ACD).
ACD is a red, itchy rash that occurs when a substance repeatedly comes into contact with skin, leading to sensitization and causing an allergic response. It is estimated to affect 20 per cent of the general population, and can be caused by many substances such as nickel and latex as well as medical substances like topical antibiotics.
The main ingredient of concern for ACD in ointments like Polysporin is bacitracin, an antibiotic, says Joel DeKoven, a Toronto dermatologist and president of the North American Contact Dermatitis Group. Some preparations contain polymyxin B, another antibiotic, and lidocaine, which numbs the skin. Both ingredients also can cause ACD, although to a lesser extent.
Bacitracin was listed as the Contact Allergen of the Year in 2003 by the American Contact Dermatitis Society to raise awareness about its association with ACD. For his part, DeKoven focuses on teaching students and physicians about ACD and common allergens like bacitracin.
It is difficult to tell how many people are sensitized to bacitracin because, as far as he knows, the only data available pertains to patients who have been referred for patch testing rather than the general population. For decades, however, it has been on the dermatitis group’s annual top 10 list of the most common allergens, as determined among patients who are patch tested.
The percentage of patch-tested patients who are allergic to bacitracin has gradually decreased from 8.2 per cent in 2009 to 5.1 per cent in 2019-2020, falling to the 15th most common allergen. DeKoven is unsure of the reason but says one possibility may be that health-care practitioners are recommending bacitracin less frequently.
At his infectious diseases clinic at Trillium Health Partners in Mississauga, Ont., Sumon Chakrabarti often sees patients with what is presumed to be a non-resolving infection but turns out to be ACD due to prolonged use of topical antibiotics. After learning about ACD from a plastic surgery colleague, he now makes sure to ask about topical antibiotic use in all his patients.
“It was crazy how many people were using goodly amounts of Polysporin,” he says.
Though the label directions advise to avoid using the ointment over large areas, in deep or puncture wounds, on animal bites or serious burns or for more than seven days, Chakrabarti says that “during the pandemic, maybe people have been applying it more to protect wounds and avoid going to the hospital that I’ve seen so much Polysporin toxicity. It ends up causing terrible wound complications. So, it’s a lot more common than I would have originally thought.”
“I’ve seen so much Polysporin toxicity. It ends up causing terrible wound complications.”
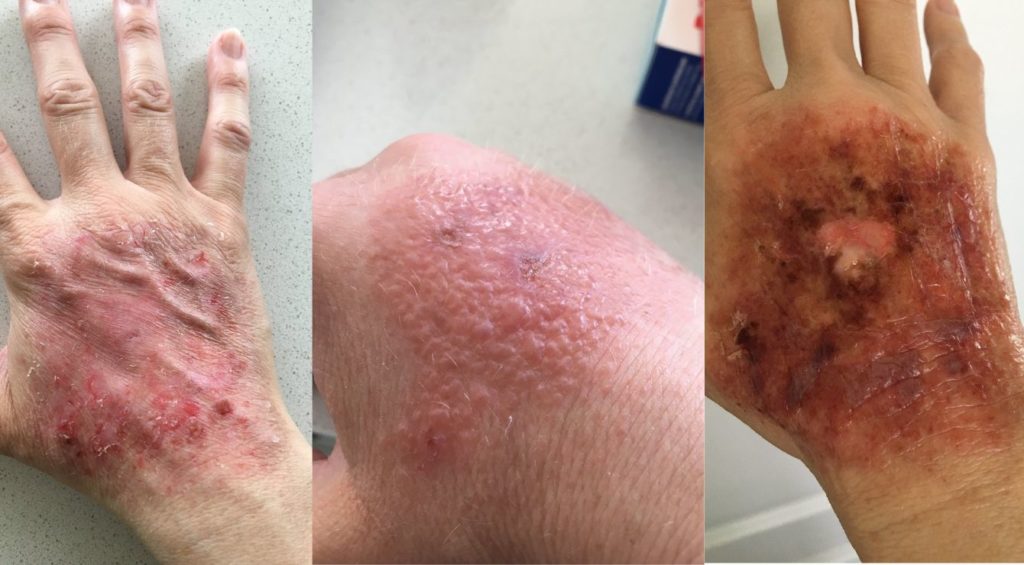
Chakrabarti sees patients who have applied antibiotic ointment to a cut or a bite, which then progressively becomes redder and inflamed and has been misdiagnosed as an infection. The patient often continues to apply antibiotics topically and is often treated with several rounds of oral or IV antibiotics without improvement. In severe cases, the skin will blister and slough. He says he remembers one patient who developed necrosis of the skin, to the point that a tendon was exposed.
“When I tell them this is probably from the Polysporin they’re putting on, a light goes off because they didn’t know,” he says. “But then all of a sudden, it makes sense.
“Obviously, there is no shaming or blaming. Polysporin is like a household name … I think there sometimes is the impression that over-the-counter drugs are totally harmless, but obviously that’s not the case.
“I appreciate as well that I’m seeing the tip of the iceberg.”
Chakrabarti adds that patients with ACD are more likely to visit a walk-in clinic or family physician’s office; researching the prevalence of bacitracin sensitization in the general population would be important to better understand this issue.
Despite growing awareness of ACD among physicians, according to the product website, Polysporin remains the “#1 doctor and pharmacist recommended anti-infective brand.”
“It’s like the kneejerk response in North America, which is all coming from marketing …” says Sandy Skotnicki, an Assistant Professor in Dermatology at the University of Toronto with an academic interest in contact dermatitis, and the author of Beyond Soap. “It’s just part of the brand, it’s like a panacea. It’ll fix everything.
“If you go to Europe, they’ve never even heard of Polysporin because it’s not really marketed there. If you go to a pharmacy in France, they’ll give you something called panthenol, which is Vitamin B5, and it has been shown to help heal wounds. And the allergies to bacitracin and polymyxin B are less in Europe.”
She advises patients against using topical antibiotics to prevent infection or speed wound healing after a biopsy, for example. Studies have shown that applying Vaseline to surgical wounds is cheaper yet as effective at preventing infection as bacitracin ointment, without the risk of ACD.
DeKoven says that while antibiotic ointments could help clear up a mild infection, he does not recommend ointments containing bacitracin because it’s a known sensitizer.
For its part, Johnson and Johnson, the manufacturer of Polysporin, said in an emailed statement: “We continually monitor our products and stand behind their safety and efficacy. Polysporin wound care products have been authorized for sale by Health Canada for more than 20 years and when used as directed, are safe and effective to help prevent infection and aid healing of minor cuts, scrapes and burns … We always recommend consumers read and follow the label.”
The label recommends to “avoid use if allergic to any of the ingredients, and to discontinue use and consult a physician if irritation occurs.”


The comments section is closed.
Hi there. I was wondering why this was happening to me. I have been tested several times to ingredients in polysporin and nothing happened. But everytime I use it I get a burned skin reaction. Usually on the 4 th day or so. I got a perscription Tara maraprin and that helps more. But may because I use less of it it’s ok? Why don’t I get a reaction to that gel? I have recently fell on my face and I used polysporin as I wasn’t supposed to use the other gel on my face and now I have a burnt like reaction on 1/2 my face. What should I do!
Excellent article.